Thank you for paving the way toward better brain health.
Winter 2024

Cormac Maher, MD
Dear Friends,
Since joining the Division of Pediatric Neurosurgery in early 2023, I have been excited to continue driving the research and innovation needed to revolutionize clinical care for our young patients.
Combining compassion with innovative research, our division is home to one of the most advanced surgical facilities in the country. Each day, we work with families to provide vital interventions for children living with the full range of brain, spine, and nerve disorders. I regard this as both a challenge and a privilege because we can fundamentally change the course of these children’s entire lives.
I am thrilled to be here at Lucile Packard Children's Hospital Stanford, and it is an honor to share this report on how your philanthropy is making a difference. We have a wonderful team in pediatric neurosurgery and great partners across departments. The sky is the limit here, and I can't wait to see what we can achieve together.
Sincerely yours,
Cormac O. Maher, MD
Botha Chan Endowed Professor
Chief of Pediatric Neurosurgery
Building a Bright Future in Neurosurgery
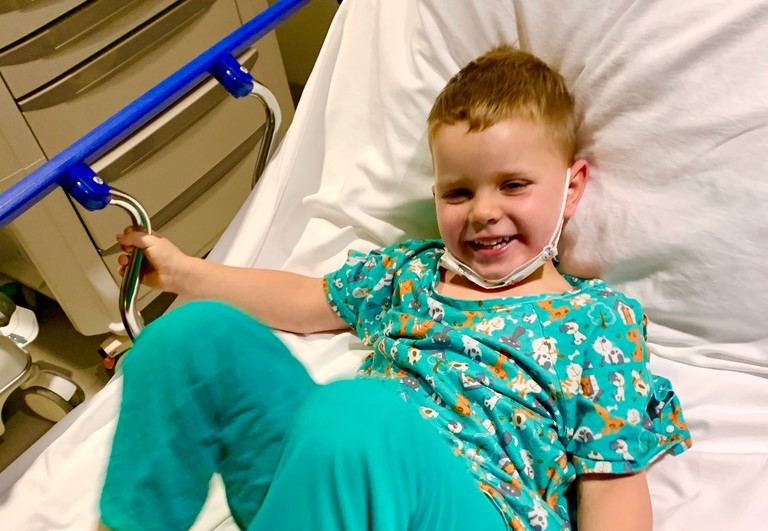
Your generosity helps kids like Carter stay in the game.
During 4-year-old Carter's very first T-ball game, he ran headlong into another child while trying to catch a ball. After a CT scan at a local hospital to check for a concussion, the family received shocking news: Carter had a brain tumor. At the urging of their physician, the family brought Carter to Packard Children's, where they met with Kelly Mahaney, MD. Carter was diagnosed with a choroid plexus papilloma—a rare kind of benign brain tumor.
Even though it was small, no one could predict if the tumor would spread. Dr. Mahaney operated on Carter, successfully removing the tumor.
Since the surgery, Carter hasn't missed a step, even playing his first season of flag football.
"Carter’s whole life has been a series of miracles," says Carter's father, Patrick. "We are filled with humble gratitude that he is a healthy, happy 4-year-old because of the generosity of donors who allow lifesaving work to be done by medical staff at Packard Children’s Hospital."

Tackling Brain Tumors from Every Angle
With every new discovery, our experts are one step closer to cures for kids like Carter. Innovative therapies, where we can tailor treatments precisely to each child's unique tumor characteristics, are right around the corner—and your partnership is propelling our research forward.
By championing the brightest minds in neuro-oncology, supporters like you empower scientific investigations like:

Curing the Uncurable
Until recently, science could offer no real treatment for a rare brain tumor called diffuse intrinsic pontine glioma (DIPG). Most patients with DIPG do not survive for more than one year, and treatment options remain limited. Now Stanford researchers, led by Michelle Monje, MD, PhD, are pioneering more effective therapies for DIPG and other deadly pediatric brain cancers.
Dr. Monje and her team have identified a molecule on the surface of these tumors to target with CAR T-cell therapy. Through this therapy, a patient's own immune cells are engineered to attack specific cancer cells—to seek and destroy the invaders. The inspiring result: the virtual elimination of brain tumors in preclinical models.
Click on the box below to read more about Dr. Monje's life-changing discoveries.
Because DIPG tumors enmesh themselves within the nervous system, these tumor cells are not just invading neural circuits in the brain. They are integrating into them electrically, structurally, and functionally, which makes them difficult to target with therapeutics.
CAR T-cell, or chimeric antigen receptor T cell, therapy is a promising form of immunotherapy designed to fight cancer. Scientists collect special immune cells, called T cells, from the patient's blood. These cells are then modified in the lab so that they act like homing devices, allowing the T cells to recognize and latch onto specific proteins on the surface of cancer cells.
The results of Dr. Monje's research using CAR T-cell to attack brain tumors are unprecedented. Patients have shown a dramatic improvement in symptoms and quality of life.
These findings give Dr. Monje hope that we are closer to having a therapy. She is continuing to refine the treatment, which she believes will ultimately transform the future for patients with many types of brain tumors.


Improving Patient Outcomes
High-grade gliomas, which are tumors of the brain and spinal cord, move fast. They spread quickly through brain tissue, and are challenging to surgically remove, making them very difficult to treat effectively.
Much of the research on high-grade gliomas has relied on treatments developed for adult patients. However, pediatric tumors are quite different. Leveraging patient tumor samples from over a decade of collection, Laura Prolo, MD, PhD, is pursuing novel treatment options tailored to pediatric brain tumors. By understanding these differences, Dr. Prolo and her team hope to identify which treatments work best for children with high-grade gliomas.
Click on the boxes below to learn more about Dr. Prolo's research.
High-grade gliomas invade surrounding tissues, spreading malignancy throughout the brain. Through lab experiments, Dr. Prolo identified specific genes that are involved with tumor cell invasion. Using the revolutionary CRISPR-Cas9 gene-editing technology, Dr. Prolo was able to "knock out" problematic genes within tumor cells. This technique effectively halted tumor cell migration and invasion in primary experiments.
Now, the research team is delving deeper into the underlying pathways and functions of these genes. They are also developing a model to test if knocking out the genes might extend survival rates. Together, these investigations hold immense potential for identifying novel therapeutic targets that could transform treatment options for kids with brain tumors.

Research has long shown that circadian rhythms—the body's daily rhythms—can have a big impact on health. A recent study further indicates that the timing of chemotherapy may have a significant impact on patient survival rates.
Building on this finding, Dr. Prolo and her team are investigating the potential influence of circadian rhythms on chemotherapy response and brain tumor behavior. This research holds the potential to improve therapeutic strategies so that kids with brain tumors can enjoy longer, fuller lives.

"We've got to make strides for patient care in the short term and find cures in the long term. Now is the time for team science and diversity of perspective."
Michelle Monje, MD, PhD
Professor of Neurology and Neurological Sciences
and, by courtesy, of Neurosurgery,
Pediatrics, Pathology, and Psychiatry & Behavioral Sciences
Making Sure Kids Everywhere Can Be Kids
At Packard Children's, we know that health care isn't just treating physical illness.
The needs of our patients extend far beyond diagnosis and treatment—kids feel best when they have the opportunity to just be kids. Your support of initiatives like food insecurity screenings and educational programs makes all the difference for patients and their families.
The partnership of donors like you ensures we can care for the whole child, and not just their disease.
Tackling food insecurity
Across the United States, nearly 9 million children experience food insecurity. Limited access to healthy foods places entire families at higher risk for diseases like diabetes, obesity, depression, and other adverse health conditions. Hungry kids also struggle to learn in school, and poor diets can make healing more difficult for children with chronic health problems.
To help combat this urgent and growing problem, our neurologists provide food insecurity screenings at every clinic visit. Families who report struggling with the rising costs of food are immediately provided with groceries. They are also connected with social workers who can direct them to additional community and government resources.

The pandemic made health disparities already present in our community even more apparent. Ensuring access to nutritious food is an essential part of health care, and we can play a role in addressing this and other barriers to improve childhood health."
Jenna Klotz, MD
This program has become a key priority across the neurology division. By making questions about food insecurity a routine part of clinic visits, our physicians aim to overcome the stigma and help families in need across our communities.
Healing the whole child
Attending school is a central part of childhood, yet many kids with neurological conditions experience ongoing cognitive effects of their illness and treatment.
Through Hospital Educational Advocacy Liaisons (HEAL), we help children engage in learning by providing support to the entire family. Through this program, our experts provide everything from neuropsychological testing, to educational assessments, to family advocacy at Individualized Education Program (IEP) meetings at school.
HEAL also works with families and school staff to understand each child's unique learning and socio-emotional needs, providing kids with the best opportunities to excel.

Each year, the HEAL program continues to expand, helping us meet the high demand for testing and advocacy services. Philanthropy like yours is critical to providing holistic and compassionate care to these children.
Thank you!
Your support for neurosurgery offers our patients the gift of hope and healing. Through your generosity, we're making remarkable strides in brain health, building a future where compassion meets cutting-edge care.
On behalf of our patients, families, faculty, and staff, we are grateful for your partnership.
For more information, contact:
Melisa Addison
Senior Associate Director, Major Gifts
(650) 461-9893; Melisa.Addison@LPFCH.org

